Breathing For Health
Written by Dr Jeffrey Kestenberg MDSc LDS FRACDS Dentist at Coburg Dental Group
There are so many things in life which we take for granted. We expect to have shelter to be protected from the elements. We expect to have the comforts of home such as a bed, a radio, a television, running water and plumbed sewerage. We consider these to be the basics of life in our society. We also expect to have food with cooking facilities and a fridge readily available and above all, we expect to have fresh air to breathe.
We can actually survive for a long time without most of these necessities but the one thing which we need every minute of every day, is fresh air. Simply, if you can’t breathe for a few minutes, you’re dead. If you breathe polluted air, you’ll be sick. And if your airway is compromised or obstructed, you will also be sick with conditions such as obstructive sleep apnoea, asthma, or emphysema. Obstructive sleep apnoea is the most common sleep-related breathing disorder.
So why is a dentist writing about this? Well, there’s been a lot of research in recent years about the dental treatment of obstructive sleep apnoea and the effect of dental and jaw growth on the function of the upper aspects of the airway. Diagnostic and treatment protocols have been developed to overcome these issues.
Sleep apnoea is a condition which should not be ignored. It can be a serious health condition. It is caused by the muscles of the tongue, soft palate, and throat relaxing temporarily. This causes narrowing or complete closure of the upper airway causing a moment when the breathing is cut off. This is known as an apnoea or hypopnoea. The classic symptoms include chronic snoring, or loud breathing during sleep, periods of no breathing during sleep, abrupt awakenings accompanied by gasping for air or choking, awakening with a sore throat or dry mouth, awakening in the morning and still feeling fatigued, morning headache, difficulty concentrating during the day, mood changes such as depression and irritability, falling asleep in the middle of the day eg at a red light while driving, while working or watching television, constantly sweating in your sleep, and decreased libido. Some people confuse obstructive sleep apnoea with chronic fatigue syndrome or insomnia. Patients with obstructive sleep apnoea are more likely to have co-morbidities such as obesity and hypertension (high blood pressure). There is also an increased incidence of cardiovascular disease and conditions like strokes, and lifestyle issues. Many serious motor vehicle accidents have drivers with obstructive sleep apnoea as a related cause of the collision.
Obstructive sleep apnoea is diagnosed by having a sleep study, known as a polysomnogram, performed in a hospital or at home. If you suspect that you have the condition your medical GP can refer you to a sleep physician or ear, nose and throat surgeon who will then arrange the sleep study to be undertaken. The sleep study measures several parameters such as breathing, incidence of snoring, incidence of apnoeas, sleep position, and oxygen levels.
Following an assessment of the sleep study, the sleep physician can classify the sleep apnoea as mild, moderate, or severe. It should also be noted that some people can snore and not have sleep apnoea.
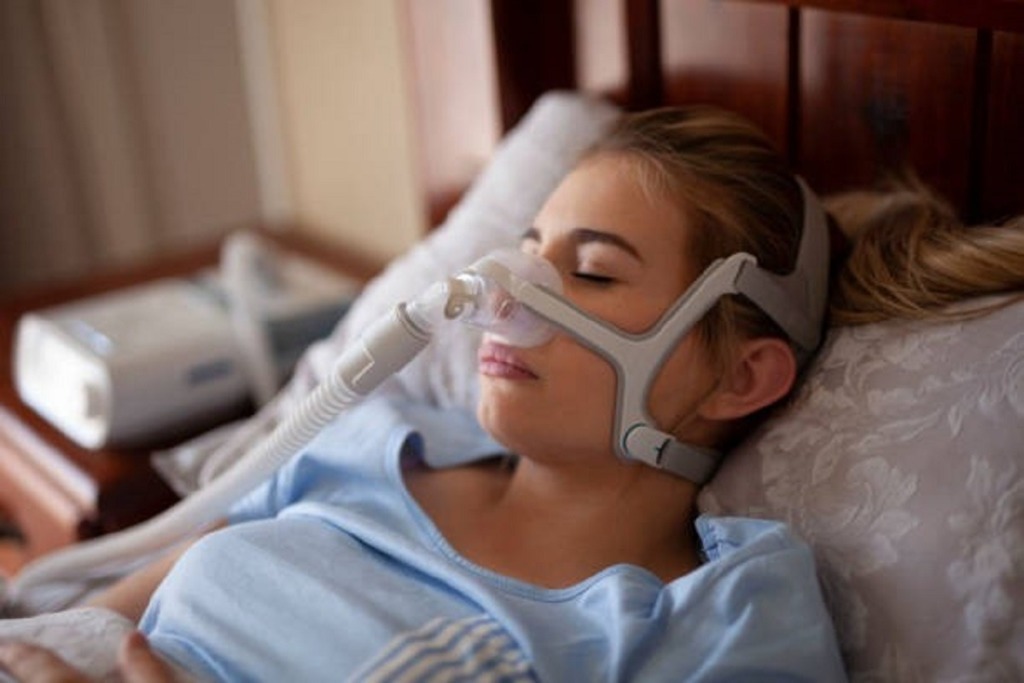
Dentists work with sleep physicians or ear, nose, and throat surgeons to provide a removable, dental plate which is worn over the teeth to treat obstructive sleep apnoea and/or stop the snoring. These plates are known as mandibular advancement splints. There are many different designs of these plates, but the best ones are customized for the patient. The plate is worn only while a patient is asleep. It is designed to position the lower jaw in a forward position to open the upper aspects of the airway which is where the obstruction is usually located. With a more open airway, more air can get into the lungs, and hence more oxygen into the blood stream and then the brain so that a more restful sleep is the end result. This is a similar end result to CPAP (continuous positive airway pressure) therapy or some surgical procedures which are the alternative treatments to mandibular advancement splints.
Like CPAP, mandibular advancement splints do not cure obstructive sleep apnoea. These treatments help to manage the condition, so that the patient can have a more normal and healthier lifestyle. These therapies need to be used in the long term and patient compliance is important for long term success.
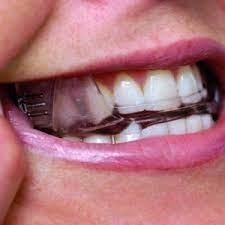
To have a mandibular advancement splint made, you require a referral from the sleep physician or ear, nose, and throat surgeon to a specially trained dentist. A referral from a GP dentist is not permitted by the Dental Board of Australia.
The dentist will then examine your teeth, gums, jaw joints and the range of motion of your lower jaw to determine your suitability to wear a splint. X-rays are also usually required as part of this initial assessment.
Once your suitability is established, the dentist will either take impressions or moulds of your teeth and a record of your jaw movement in a forward direction or will make a digital scan of your teeth and jaw movement. The scan is more comfortable, accurate and can be easily stored and reproduced for future use if required.
A dental laboratory will then use the impressions or the digital scan to make a customized, mandibular advancement splint by freehand (known as an analogue appliance) or 3-D printed (a digital appliance). The appliance is then issued to the patient to be worn every night.
Most of the good, modern splints can have the ability to vary the amount of forward jaw movement and to allow the opening of the mouth for patient comfort. These appliances can be adjusted for comfort and easily repaired if broken. Dental health issues such as tooth decay, inflamed gums, loose teeth, broken fillings and crowns will need to be rectified prior to the splint being made.
Success rates of splint therapy treatment do vary according to the study and the severity of the initial condition but often clinicians quote a success rate of 80% in reducing the incidence of the symptoms to a relatively normal level and returning the patient to a normal lifestyle.
Any surgical or invasive procedure carries risks. Before proceeding, you should seek a second opinion from an appropriately qualified health practitioner.